Five months ago, 2-year-old Xiao Qiang was admitted to hospital with recurrent fevers, and a devastating diagnosis shattered his family—he had a nephroblastoma in his right kidney. Like a wildly spreading vine, the malignant tumor snaked from his right kidney along the blood vessels, through the inferior vena cava, and finally into his beating right atrium. Local hospitals could do nothing to help. His parents took him on a desperate journey across Henan and Shandong provinces, undergoing 8 rounds of chemotherapy, yet the tumor’s advance never slowed. When they arrived at Beijing Jingdu Children's Hospital clinging to their last hope, despair was etched deep in their eyes.
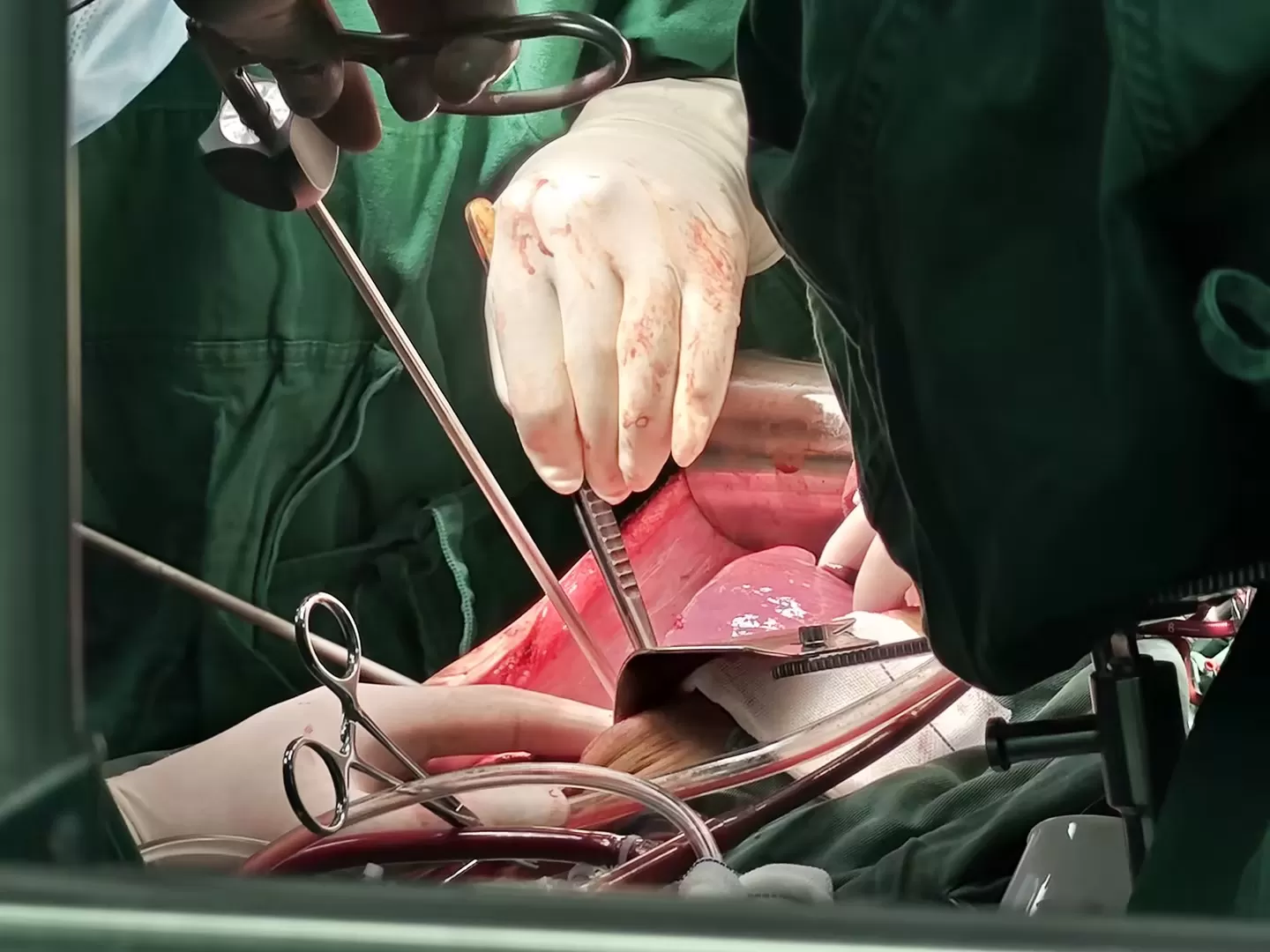
If the human inferior vena cava and atrium are likened to a high-speed, high-pressure water pipe, the tumor thrombus in the heart is a bomb primed to detonate at any moment. The inferior vena cava and atrium are the main thoroughfares for blood return in the human body, where blood flows at high speed and pressure. What the doctors had to do was extract this "poison vine" in one piece—without breaking the "pipe" or shattering the "bomb"—and rebuild blood flow with a "spare pipeline" (allogeneic blood vessels). A single tiny mistake could trigger catastrophic bleeding (a "pipe burst"), pulmonary embolism (from "bomb shrapnel flying"), or the spread of tumor debris, killing the child instantly.
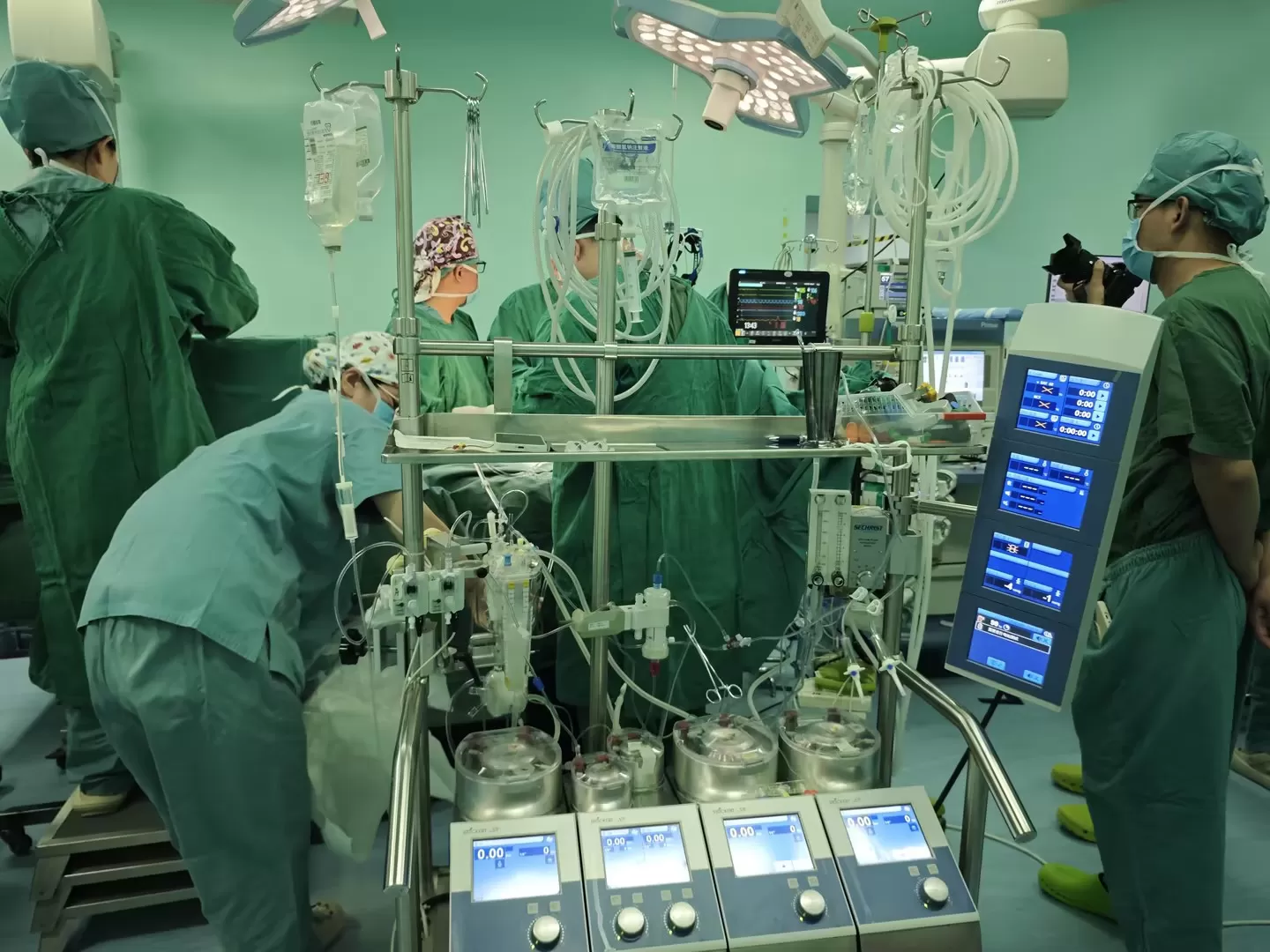
Anatomical complexity: The tumor thrombus spanned the abdominal and thoracic cavities and invaded the right atrium, requiring a combined abdominal and cardiac approach with cardiopulmonary bypass (CPB) support to temporarily take over heart function and create a bloodless, safe surgical field. It also demanded close collaboration among specialists from cardiac surgery, abdominal surgery, vascular surgery, urology, and anesthesiology.
Reconstruction difficulty: The renal blood vessels, hepatic veins, and inferior vena cava were severely invaded, requiring an estimated 4 to 5 vascular anastomoses. Each additional anastomosis doubled the surgical risk, and the failure risk of 4 to 5 anastomoses increased exponentially. Meanwhile, allogeneic vascular transplantation for major vascular reconstruction placed extreme demands on anastomotic techniques and postoperative management.
Organ hypoxia risk: The core challenges included controlling massive bleeding in the child’s hypovolemic state, preventing pulmonary embolism from tumor thrombus dislodgement, and guarding against ischemia-reperfusion injury to the brain, kidneys, and multiple organs. Inadequate anesthetic technique would have meant the child might never wake up. Specialized equipment was therefore used intraoperatively to monitor oxygen perfusion levels in the brain, kidneys, and lungs.
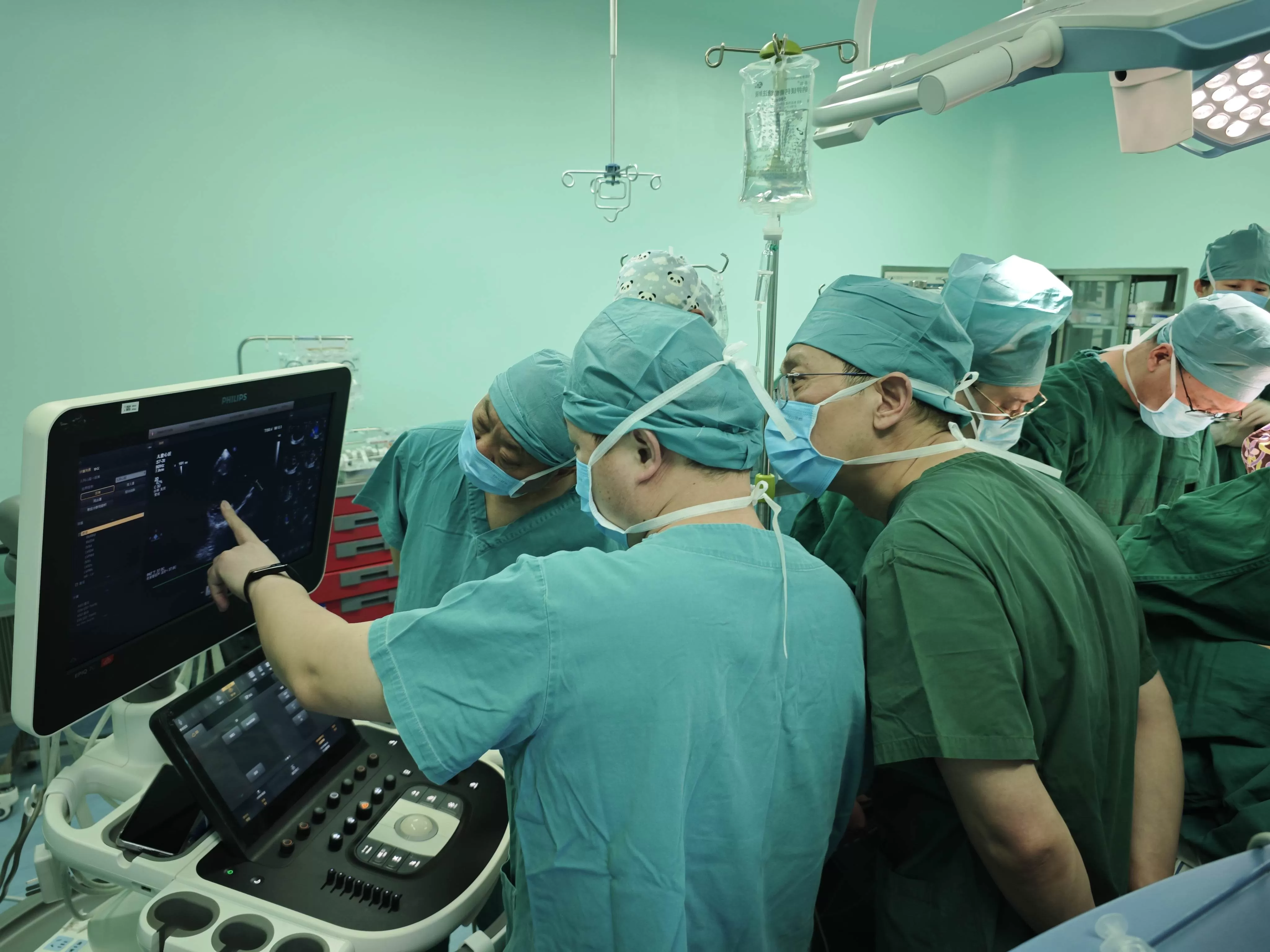
This surgery was as difficult as performing 5 top-tier cardiac surgeries at once—requiring precise completion of 5 vascular anastomoses, each demanding the meticulous precision of embroidery, where the slightest error leads to disastrous consequences. To conquer these challenges, the International Children's Cancer Center at Beijing Jingdu Children's Hospital activated a multidisciplinary team (MDT) approach. Specialists from pediatric oncology surgery, cardiac surgery, vascular surgery, anesthesiology, radiology, and critical care medicine jointly developed a treatment plan, assembling a "medical task force" of 12 experts from 7 departments.
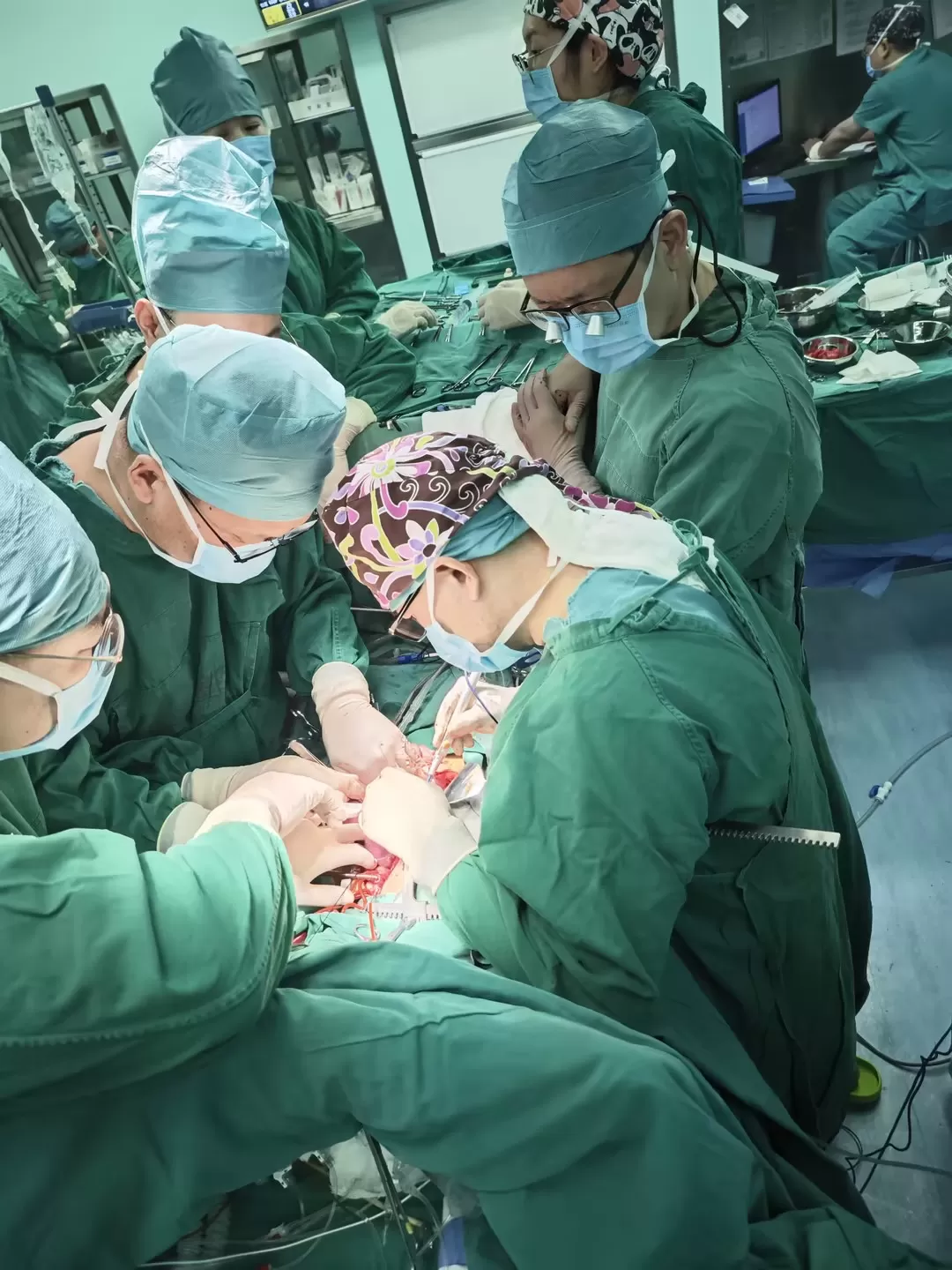
Intraoperative monitoring: Transesophageal echocardiography (TEE) was used throughout the procedure to visualize the heart in real time via an esophageal probe, accurately localizing the lesion and preventing tumor dislodgement and systemic spread caused by surgical manipulation.
Cardiopulmonary bypass technology: CPB was administered to control cardiac pressure and enable safe thrombus extraction.
Surgical approach: A combined midline abdominal incision and median sternotomy were adopted. Proximal blood vessels were first controlled, the right atrium was incised under deep hypothermic low-flow perfusion, and the tumor thrombus was removed intact.
Precision reconstruction: Overcoming the challenge of the child’s tiny vascular calibers, the surgical team resected multiple segments of affected blood vessels and performed allogeneic vascular replacement, completing 5 high-quality vascular anastomoses to ensure hemodynamic stability.
Cerebral protection: Cerebral monitoring equipment was used to track cerebral blood flow and oxygen levels, safeguarding the brain.

The chief surgeon is a leading expert in pediatric oncology surgery in China, having led the completion of multiple Asia-first high-difficulty surgeries. He and his team repeatedly refined the surgical plan and conducted more than a dozen simulation exercises to ensure every step was flawless. The surgery lasted a full 10 hours—far longer than a typical general surgery (which usually takes 1 to 3 hours)—meaning 12 specialists worked at an intense pace for an entire workday, without a moment’s slack. At the 6th hour of the operation, the tumor thrombus was completely extracted from the heart, and the right renal tumor and the invaded inferior vena cava were resected en bloc. When the 5th anastomosis was finished, blood flowed smoothly again and the beating heart returned to a steady rhythm, sending a wave of elation through the operating room. After the surgery, the child was transferred to the pediatric intensive care unit (PICU), where a dedicated medical team provided 24/7 monitoring to lay a solid foundation for postoperative recovery.
Hearteningly, on the third day after surgery, Xiao Qiang regained consciousness smoothly, opened his eyes, and whispered "Mom". His vital signs were stable, and his parents, waiting outside the PICU, wept tears of joy and hugged each other tightly. This life-and-death battle had ended in victory. Although the child still needs to complete adjuvant chemotherapy, radiotherapy, and immunotherapy in the hospital, the successful removal of the tumor has made all subsequent treatments possible—and hope for a cure a reality.
As one of the few children’s cancer centers in China capable of performing such high-difficulty surgeries independently, the International Children's Cancer Center at Beijing Jingdu Children's Hospital adheres to internationally aligned diagnosis and treatment standards and maintains close academic exchanges with top children’s cancer centers in the United States and Europe. Boasting the expertise to perform cutting-edge surgeries and a comprehensive treatment system, it treats a wide range of pediatric cancers including neuroblastoma, hepatoblastoma, nephroblastoma, and rhabdomyosarcoma. Each year, it provides standardized treatment for 1,200 patients, with cure rates for many pediatric cancers reaching the highest international level. It has become the last hope for cancer-stricken children and their families worldwide.